Gynaecomastia (Male Breast Reduction)
Gynaecomastia, or “moobs” as it is sometimes referred to, is the medical term for female breast that develop on a male. This can occur from any age but is more common after puberty and can result from a number of causes including being overweight, taking steroids, marijuana usage, hormonal causes as well as a genetic predisposition to name only a few – you should have this investigated by your GP before coming to discuss possible surgical correction. The tissue can be comprised of mainly breast tissue, mainly fat or a combination of the two. It can sometimes only affect one breast. Enquire now for male breast reduction in Hertfordshire.
Gynaecomastia
- Have breasts resistant to weight loss
- have ptotic (droopy) breasts
- wish to try to improve any asymmetry in breast shape and position on the chest wall
- are not happy with the shape of their breasts
- want to improve self-image and esteem and to be able to wear tighter fitting garments
The operation is usually carried out under a General Anaesthetic (you are asleep) and takes around an hour and-a-half to complete. Several different options are available to treat the excess tissue and which one recommended will depend upon the type of tissues causing your breasts and, if applicable, the amount of loose skin to be removed. These methods include:
- Liposuction – via small ‘stab’ incisions the excess fat is removed by way of liposuction. This method does not deal with any breast (glandular) tissue present.
- Excision – A cut is made around the bottom half of the nipple areolar complex and through this the breast tissue is removed.
- Levick ‘avulsion’ technique – via an incision in the fold at the front of your armpit the fat is removed by liposuction and the breast tissue is avulsed leaving no visible scars on the breast.
The technique employed to give you the best results will be discussed with you by Mr Davis in clinic.
If you are having the Levick technique you will be required to stay in hospital for 1 night, but with the other techniques you can usually go home the same day as the surgery – occasionally a single night in hospital is advised depending upon multiple factors such as your overall medical health, distance to home from the hospital, who is at home with you etc. – this will again be discussed and agreed upon in clinic when you consult with Mr Davis.
You will be required to wear a tight fitting compression vest (Mr Davis advocates LipoElastic® garments) for a period of six weeks. If you undergo the Levick technique, you will not only be wearing compression garments but also for the first night after surgery you will be wearing a cooling dressing so as to minimise the chance of bleeding post-operatively.
You are encouraged to shower twenty-four to forty-eight hours after surgery however only using cool/tepid water temperature, either dabbing your chest dry, letting it dry naturally or to use your hairdryer on a cool setting to blow it dry – you are NOT to rub your chest for one month after surgery. You will also be asked to avoid anything that causes your blood pressure to rise for the first two weeks after surgery and will be required to abstain from physical exercise for at least 6 weeks after surgery.
A period of at least two weeks off work is advised, depending upon your job. This will be discussed further in clinic during consultation as appropriate.
After two weeks you will be asked to apply moisturiser over your scars on a daily basis for a period of three months.
You will come for a wound check one week after your surgery and return to see Mr Davis in clinic between four and six weeks after surgery, and again after three months. Further follow-ups will be arranged as necessary.
Bleeding & Haematoma
Bleeding can occur at any time in the first 10 days or so after the surgery so you should therefore avoid any trauma to your breast area and avoid strenuous exercise or anything that is causing your breasts to be moving vigorously in any direction. Where possible, arm movements should be limited in the first week.
Your breast will usually become swollen and tender with a bleed and may develop bruising – if this occurs you should return for review as you may require a return to the operating theatre to explore and stop any bleeding vessel(s)and remove any blood.
Seroma
This is a collection of clear/pale yellow fluid that essentially leaks and collects from the tissues as part of the normal reaction to surgery/injury. This nearly always resorbs over a period of weeks, but is occasionally large enough to warrant it being aspirated with a needle and syringe in clinic.
Infection
Whilst not common, should it occur your breasts may be swollen, red, warm/hot and tender – not to be confused with the inflammation of healing. You may also feel unwell in yourself. This is treated with a 5-to-7 day course of oral antibiotics. Very occasionally an infection can result in part(s) of the wound coming apart – this is managed by a regular change of dressings and showering, and will be allowed to heal by itself over the subsequent four-to-six weeks.
Swelling &/or bruising
Swelling will almost certainly occur naturally and can take months to fully settle down. Bruising can be treated, unless contraindicated, with the use of Arnica or other such products should you wish.
DVT/P.E.
Very occasionally a blood clot may form in one of the deep blood vessels in the leg (Deep Vein Thrombosis). Blood clots have the potential to break bits off that can travel up to the lungs resulting in a pulmonary embolus. As a way of reducing the risk you will be required to wear compression(TED) stockings on your legs from admission on the day of surgery until 2 weeks after surgery. You will also be encouraged to keep as mobile as is possible and to stay well hydrated.
Scars
Scars are by definition permanent, so will always be there. Initially scars can be red and with time should fade through pink to ultimately be pale and flat. Occasionally scars can become hypertrophic or keloid whereby they are raised, red, lumpy, itchy and unsightly or can stretch to become wider.
Altered nipple sensation – numb or over-sensitive
The nerves supplying the nipple areolar complex can be damaged during the surgery resulting in your nipple(s) feeling numb after surgery. This usually recovers with time, however permanent loss of or reduced sensation can happen. Ever so occasionally the nipple can become oversensitive.
Inability to breast feed
It is not uncommon to be unable to breast feed after a breast uplift as the milk ducts and/or nerve supply to them is interfered with when relocating the breast tissue.
Altered breast sensation/numbness
As per the nipple, nerve damage can occur to the nerves supplying the skin over the breast. This is usually temporary but can occasionally be permanent, resulting in numb skin.
Nipple loss – full or partial
Just as the nerves to the nipple can be damaged, so can the blood vessels that supply and keep the nipple areolar complex alive. Damage to these can result in some (partial) or all (full) of the nipple and areolar being lost.
Asymmetry
No two breasts are ever completely symmetrical – they are “sisters not twins”. Despite best efforts to make the breasts as symmetrical as is possible, minor asymmetries will remain after surgery. Very occasionally a notable asymmetry can occur that requires further surgery to adjust volume, shape or nipple position.
Fat necrosis &/or lumpiness
When the breast tissue is mobilised its blood supply can become compromised, as per the nipple, resulting in some fat and breast tissue dying off (necrosing). This presents itself as a firm lump or lumpiness within the breast, and will usually settle by itself over the subsequent months. Very occasionally the old liquid fat can discharge itself through a hole in the scar/wound, requiring regular dressings until it settle sand heals itself. Very occasionally the fat will calcify requiring further surgery to excise it.
Skin necrosis
Very rarely the blood supply to the skin of the breast can be compromised resulting in skin dying – this is most common at the T-junction where the vertical element of the scar meets the horizontal aspect of the scar in your breast crease. This is managed, should it occur, with dressings until healed. Very occasionally the scar requires revising.
Wound breakdown
Very occasionally some of the wound can come apart for a multitude of reasons. This is almost always small enough to manage conservatively with dressings, allowing nature time to heal the area. Should any scar that forms be unsightly or an issue then this can always be revised at a later date, often under a local anaesthetic such as those used by the Dentists if putting your teeth to sleep for a filling etc.
‘Dog ears’
These are little areas of skin and underlying fat/tissue that cause skin at the ends of your scars to sit a little proud. Often these settle with time and massage however occasionally they require removing under a local anaesthetic.
Further surgery in the future
This is likely to incur more costs
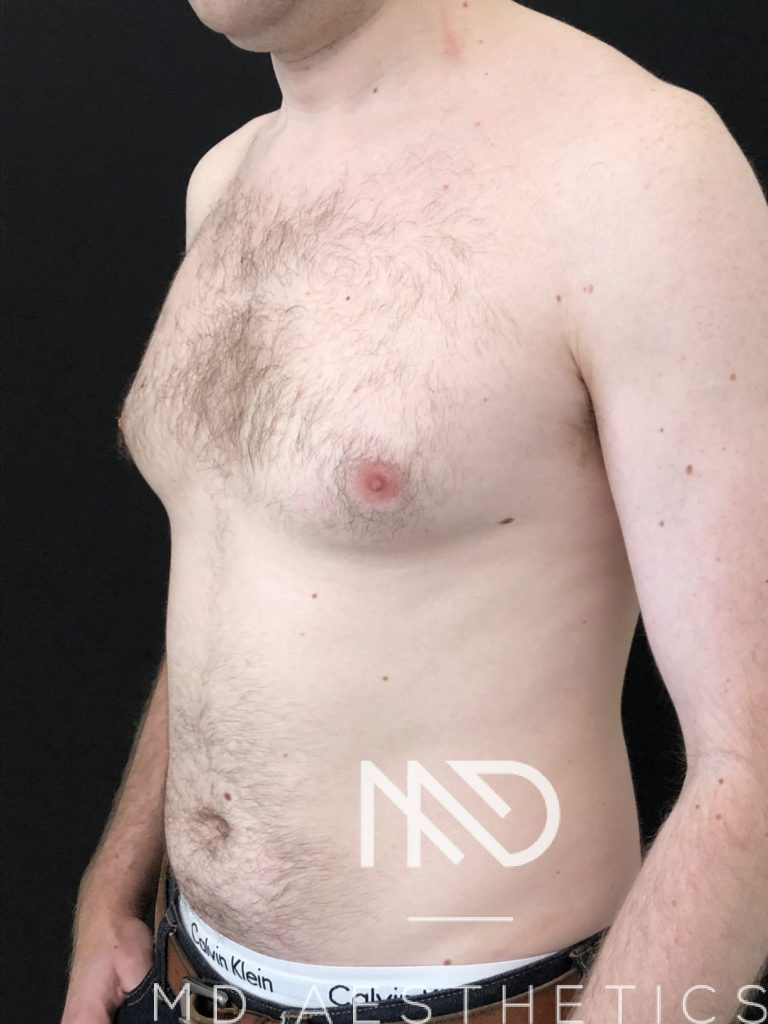
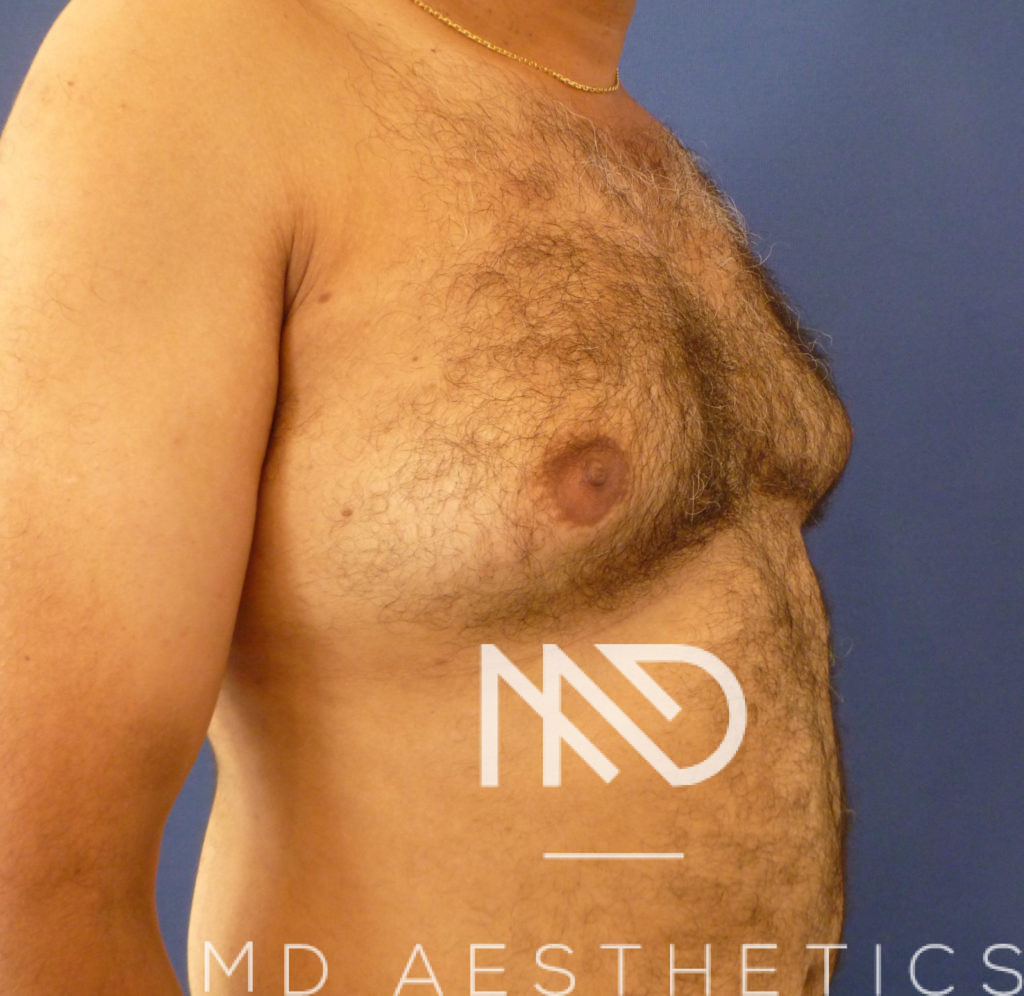
Before/After Pictures